The COVID-19 pandemic has necessitated a myriad of changes in healthcare delivery. For months, elective surgeries were delayed to focus personnel and resources on caring for coronavirus patients. Many people stayed away from emergency departments, too, or postponed important medical tests, to reduce their potential exposure to the virus. Now, with the arrival of multiple COVID vaccines and no major surge of infections, individuals are beginning to feel safer about scheduling orthopedic and other elective surgeries. They’re moving forward with medically recommended procedures. They are also more willing to seek care in a hospital emergency room.
While it seems we’re trending in the right direction, risks to medical professionals conducting surgeries or procedures - whether emergent or not - still remain. Let’s take a look at the decline and resurgence of both emergency and non-emergency aerosol-generating surgeries and procedures – and how providers can be safer from now on.
Deferred Care = Backlogs, Delays
On March 18 of last year, CMS announced that “all elective surgeries, non-essential medical, surgical, and dental procedures be delayed during the 2019 Novel Coronavirus (COVID-19) outbreak.” The decision to restart them was left to state and local governments, as well as physicians and patients1. By October 2020, McKinsey & Company predicted that hospitals and health systems would need nearly 20 months to clear the surgical logjam built up during 20202. The statistics behind that pent-up demand are all too real:
- Almost 84 percent of U.S. orthopedic procedures were delayed, postponed or canceled once the pandemic began.3
- The number of cataract surgeries went down by 97 percent, and glaucoma procedures decreased by 88 percent.4
- Average weekly colorectal cancer screenings declined by 86 percent.5
- The COVID-19 outbreak caused at least 198,000 active U.S. dentists and dental specialists to basically shut down their practices.6
Hospital and Emergency Room Safety Were in Doubt
With actual and suspected cases of COVID-19 flooding hospitals and their emergency departments as the pandemic surged, it’s understandable that people with other illnesses or injuries – and even some significant symptoms – hesitated to seek medical care in those settings. In a single month early in the pandemic, March 29-April 25, 2020, emergency department visits went down 42 percent from the same period in 2019. Those who did go to the ED were much more likely to be there due to “exposure, encounters, screening, or contact with infectious disease.”7 By August of last year, JAMA Internal Medicine was urging physicians and public health officials to remind patients that many emergencies cannot be treated in another setting, and going to an ED for any injury, illness or serious symptoms is the best course of action.8
The ways in which COVID-19 is spread was behind all the declines in surgeries, procedures and ED visits. Between transmission via direct contact, airborne droplets and to a lesser extent, contaminated surfaces, patients and practitioners felt extremely vulnerable – and rightly so.9
Prepare for a Different Kind of Surge
Although elective surgeries, preventative procedures, and emergency department visits for urgent care are on the rise, the pandemic is not over! How do you protect doctors, nurses and technicians during both emergency and non-urgent intubations, extubations and other aerosol-generating procedures (AGPs)? The CDC recommends the following:
- Provide all healthcare personnel (HCP) in the room with an N95 or higher-level respirator, eye protection, gloves, and gown.
- Limit HCP to those essential for patient care and procedure support.
- Conduct AGPs in an airborne infection isolation room (AIIR) when possible.
- Employ vacuum shrouds for surgical procedures if available.
- Clean and disinfect procedure room surfaces promptly.10
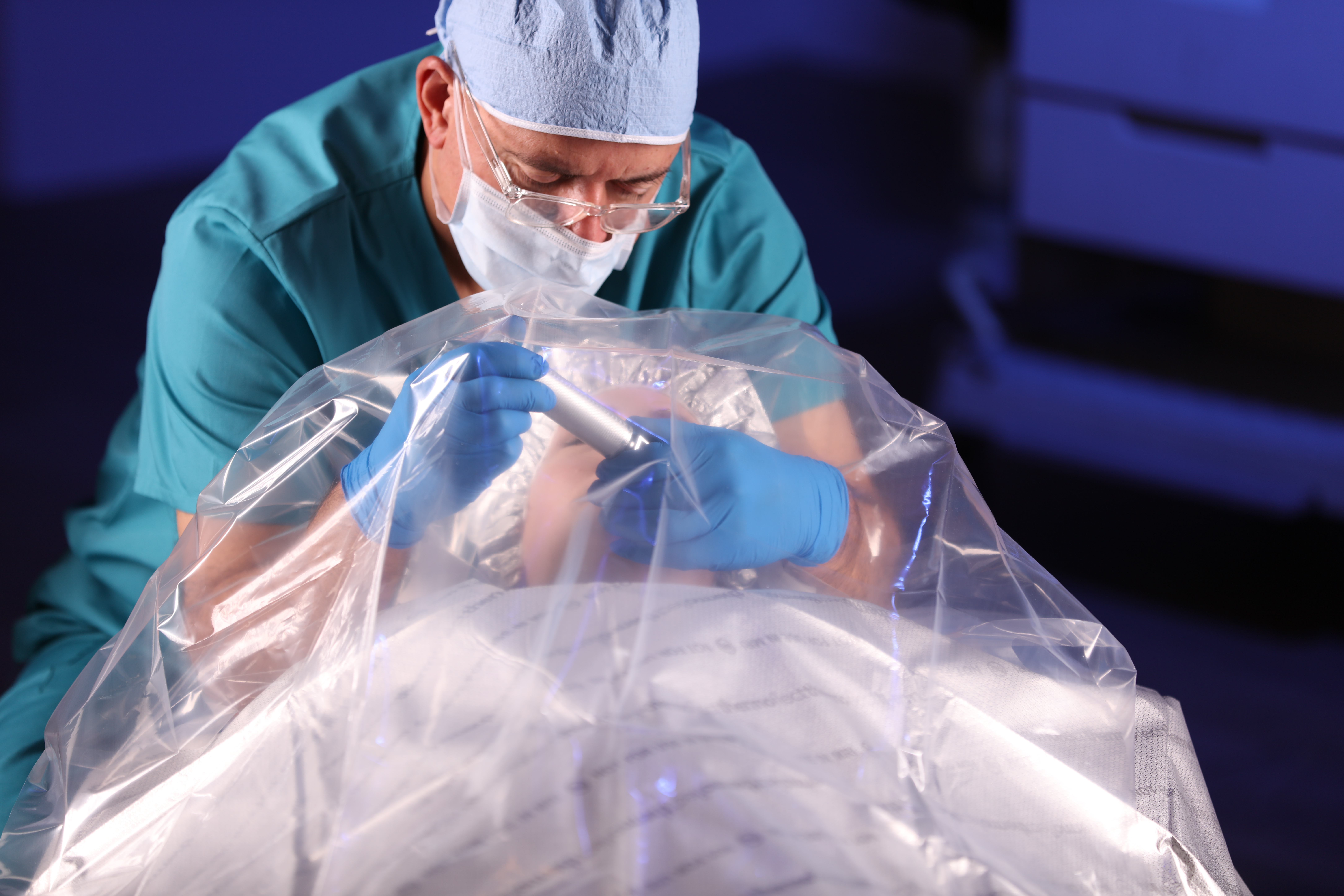
There’s another solution that adds peace of mind in surgery suites, emergency departments and procedure rooms. Our COVAIRE™ aerosol barrier protects HCP from possible pathogen exposure so they can focus on their work. By tenting the entire patient, the clear drape provides extra risk mitigation for every person in the room. It’s easily stored on a crash cart, or in an operating or procedure room, then thrown away after use. The provider has full range of motion to perform the surgery or procedure, with no workflow interruption.
From now on, think about what you can add to your infection prevention arsenal. The stakes are so much higher for ensuring the well-being of your medical staff.
References
- https://www.cms.gov/newsroom/press-releases/cms-releases-recommendations-adult-elective-surgeries-non-essential-medical-surgical-and-dental
- https://www.mckinsey.com/industries/healthcare-systems-and-services/our-insights/cutting-through-the-covid-19-surgical-backlog#
- https://www.prnewswire.com/news-releases/impact-of-covid-19-on-elective-procedures-in-the-united-states-2020-report---nearly-83-5-of-all-orthopedic-procedures-performed-have-been-delayed-postponed-or-canceled-301211703.html
- https://westbanksurgery.com/news/eye-exams-and-procedures-delayed-by-covid-19-could-result-in-vision-loss
- https://www.gastrojournal.org/article/S0016-5085(20)34932-5/pdf
- https://psnet.ahrq.gov/primer/covid-19-and-dentistry-challenges-and-opportunities-providing-safe-care
- https://www.cdc.gov/mmwr/volumes/69/wr/mm6923e1.htm#:~:text=NSSP%20found%20that%20emergency%20department,%2C%20females%2C%20and%20the%20Northeast
- https://jamanetwork.com/journals/jamainternalmedicine/fullarticle/2768777
- https://www.cdc.gov/coronavirus/2019-ncov/prevent-getting-sick/how-covid-spreads.html
- https://www.cdc.gov/coronavirus/2019-ncov/hcp/infection-control-recommendations.html