By Kristy Warren Director,
Clinical Resources Encompass Group, LLC
Pressure Injuries (PIs) and wounds have presented a significant risk to patients and a clinical challenge to nurses and other clinicians since before nursing became a profession. The skin is the largest organ of the body and although it doesn’t get the same attention as the heart, brain, liver, and lungs, it can be the most serious threat to a patient’s survival or at the very least, to their comfort and well-being. Painful localized skin injuries, called Pressure Injuries (PIs) can develop from prolonged pressure over bony areas of the body. Caring for PIs can be challenging and time-consuming for nurses and other caregivers. Severely advanced injuries can penetrate the full thickness of the skin tissue to the depth of several centimeters, exposing underlying muscle and other structures such as tendon and bone.
While the most recently published AHRQ report data for the period 2014-2017 shows an overall decrease in Hospital-Acquired Conditions (HACs), the good news from this report doesn’t extend to PIs. The rate of PIs rose by 6% over the study period. In patient terms, this uptick represents an increase of 119,000 pressure wounds, resulting in close to 5000 deaths. In addition, the average lengths of hospital stay is more than double for patients who acquire PIs during their care. Pressure injuries increase health care utilization and medical management, costing the US healthcare system around $11 billion per year.
As our population ages, the risks associated with developing a pressure injury increase. Additionally, surgical patients who may not have presented as at-risk for PIs prior to surgery, have an increased risk during surgery and post-operatively of developing a pressure injury. While not all Hospital-Acquired Pressure Injuries (HAPI) can be prevented, caregivers are able to ward off many of them by adhering to best practice standards such as those outlined in the National Pressure Injury Advisory Panel(NPIAP)/European Pressure Ulcer Advisory Panel (EPUAP) International Guidelines.
Nurses will quickly tell you that they would much rather find effective solutions to preventing pressure injuries than watch their patients suffer from painful complications. As frontline caregivers, nurses have used their insight and invention over the years to help reduce harmful hospital-acquired conditions with innovative patient-care techniques. Today’s nurses are well-positioned to take the lead in implementing care practices that will ultimately reduce the unnecessary cost and suffering caused by pressure injuries.
Addressing the many facets of PI prevention requires a collaborative approach by a multidisciplinary clinical team. Each patient should be assessed upon entry to the hospital. If the patient is deemed at risk for the development of a PI, actions to mitigate this risk should be taken immediately. The use of a multifunctional therapeutic support surface can be beneficial in alleviating pressure-related risks to the patient.
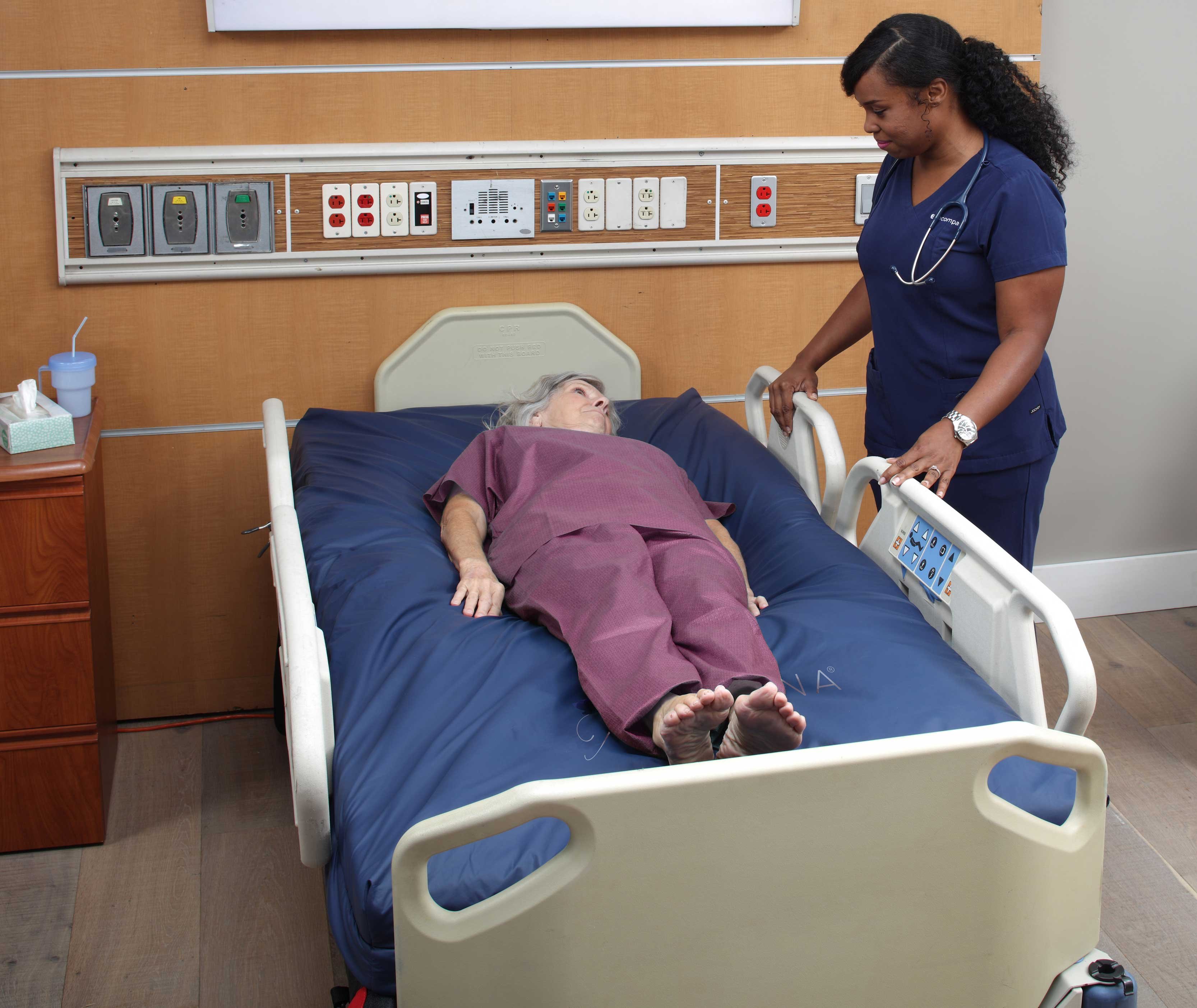
Support surfaces also known as a mattress or bed, are used to redistribute pressure on skin and subcutaneous tissue or alternate parts of the body exposed to pressure. These surfaces are made of various components including air, gel, water, and various types of foam. Support surfaces may have additional features such as alternating pressure, air fluidization, low air loss, multi-zones, turn assist, or lateral rotation. When selecting a support surface, consider the patient’s level of immobility and inactivity, the need for shear reduction, and microclimate management. Selection should include a surface with a perimeter that has firm foam boarders for stability during ingress/egress. According to research, 51% of falls occur when getting into or out of bed. Other considerations include comfort, size, weight, and the risk for PI development as well as the severity and location of existing PIs. Implementation of the correct surface should be expedient.
Many therapeutic support surfaces that are initially beneficial increasingly lose the ability to prevent PIs over time. This phenomenon generally occurs as the patient’s body tends to acclimate to the therapy setting. This adaption process, known as allostasis, will eventually slow the healing process. Another obstacle caregivers may encounter is the traditional therapeutic support surfaces and pressure injury treatments may not be well suited to the needs of collaborative members of the disciplinary team. For example, if a patient is unable to sit on the edge of the bed due to a lack of support or firm side perimeter to receive physical therapy. More than 90 percent of people being treated for PIs are also receiving care for other medical conditions. It is important to keep in mind all care disciplines when focusing on injury prevention and treatment selection.
In addition to a full line of support surfaces that are made in the USA, Encompass Group LLC recently launched the innovative, engineer, and clinician-designed AirisanaTM. AirisanaTM features the first of its kind, five support surfaces in one. This surface offers low air loss with targeted air flow, pressure redistribution, alternating pressure on a randomized cycle to prevent acclimation, microclimate management, immersion and envelopment, and lateral rotation to assist with caregiver turn assist, pulmonary health, and early mobility.
Pressure injuries in the healthcare environment are a significant problem. Guidelines consistently support the use of pressure redistribution surfaces, which provide therapy with or without the addition of alternating pressure therapy. Pressure can be minimized or mitigated by the utilization of a specialized support surface. The selection of a specific support surface should be based on the assessment of the clinical characteristics or condition of the patient and support surface characteristics. Incorporating the specific needs of the patient in the care planning will help ensure the most effective clinical outcome possible.
Stop by booth #350 at WOCNext 2022 for more information on how to take a proactive approach to pressure injury prevention!