

How Nurses Lead the Way in Reducing Pressure Injuries




Clinicians: Our Healthcare Innovators
Nobody understands the demands of healthcare better than clinicians on the frontline. Over the years, they’ve used their insight and invention to help reduce harmful hospital-acquired conditions with innovative patient-care techniques. In the same way they impacted patient care with these notable achievements, shown below, what if the same insight and invention could be used to significantly address and impact Pressure Injuries acquired in healthcare settings? Now, Encompass Group, in consultation with medical engineers, biologists, clinicians and WOC nurse professionals, has developed the patent pending AirisanaTM Therapeutic Support Surface, with a desire to make that “what if?” a reality.

The Kenny Method
Elizabeth Kenny pioneered an alternate approach to treating polio called The Kenny Method. It was based on her deductions that the physical manifestation of polio was caused by a viral infection of muscle and other peripheral tissue. This countered the common thinking that it was caused by an infection of the nervous system. Scientists later demonstrated she was right!
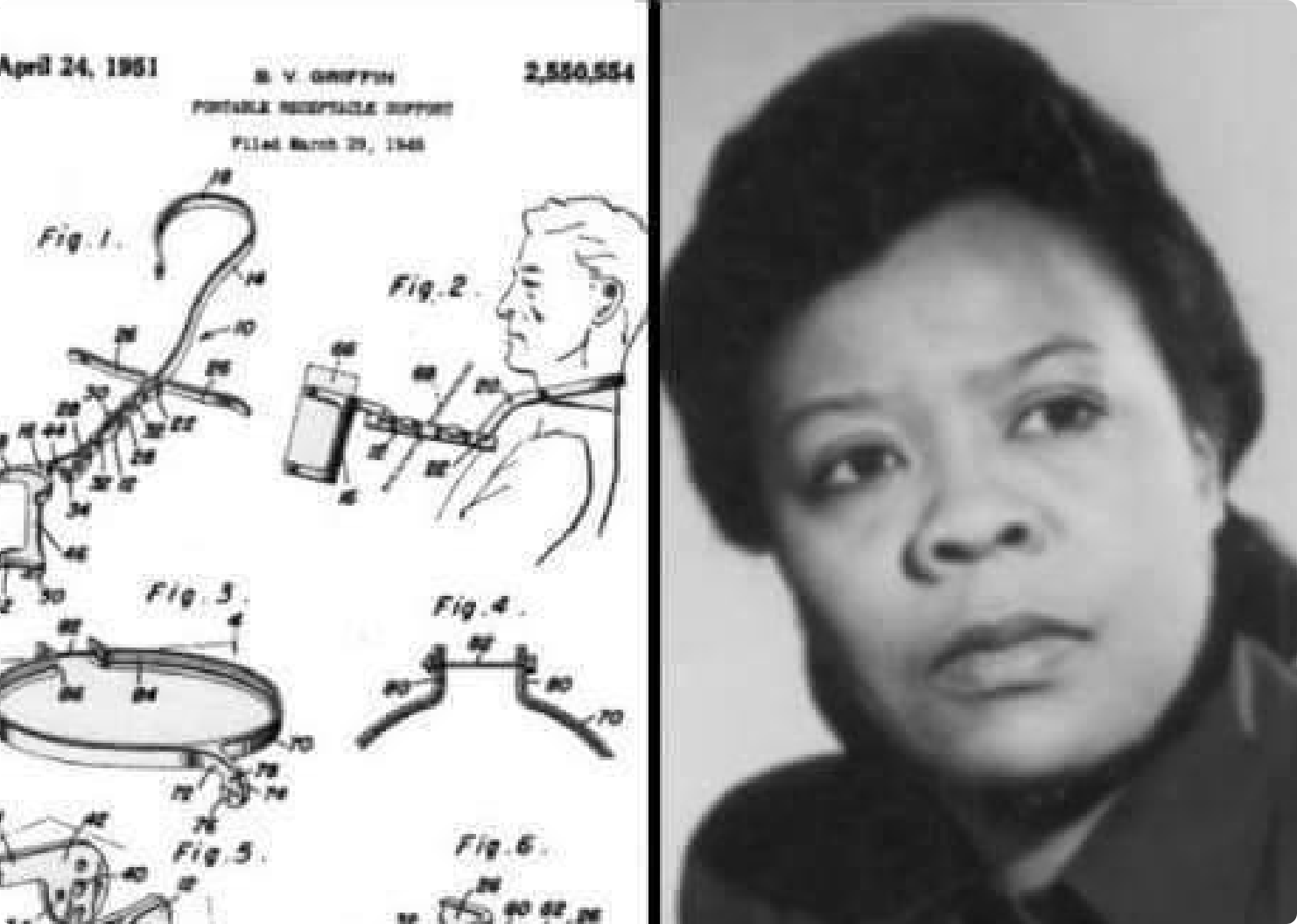
Feeding Tubes for Veterans
n the 1940s, Bessie Blount Griffin noticed how paralyzed WWII veterans and amputees were often unable to feed themselves. She invented a tube they could use with their teeth to give them back a measure of independence. This was only one of her many innovations — she also pioneered the field of medical graphology!

The Ostomy Pouch
Danish clinician, Elise Sorensen, invented the ostomy pouch by pioneering the use of a plastic pouch that could adhere to a patient’s body. Motivated to help colostomy patients after her sister had the surgery at age 32, she went on to be elected nurse of the year in 1963 by The Danish Nurses’ Organization for her efforts.
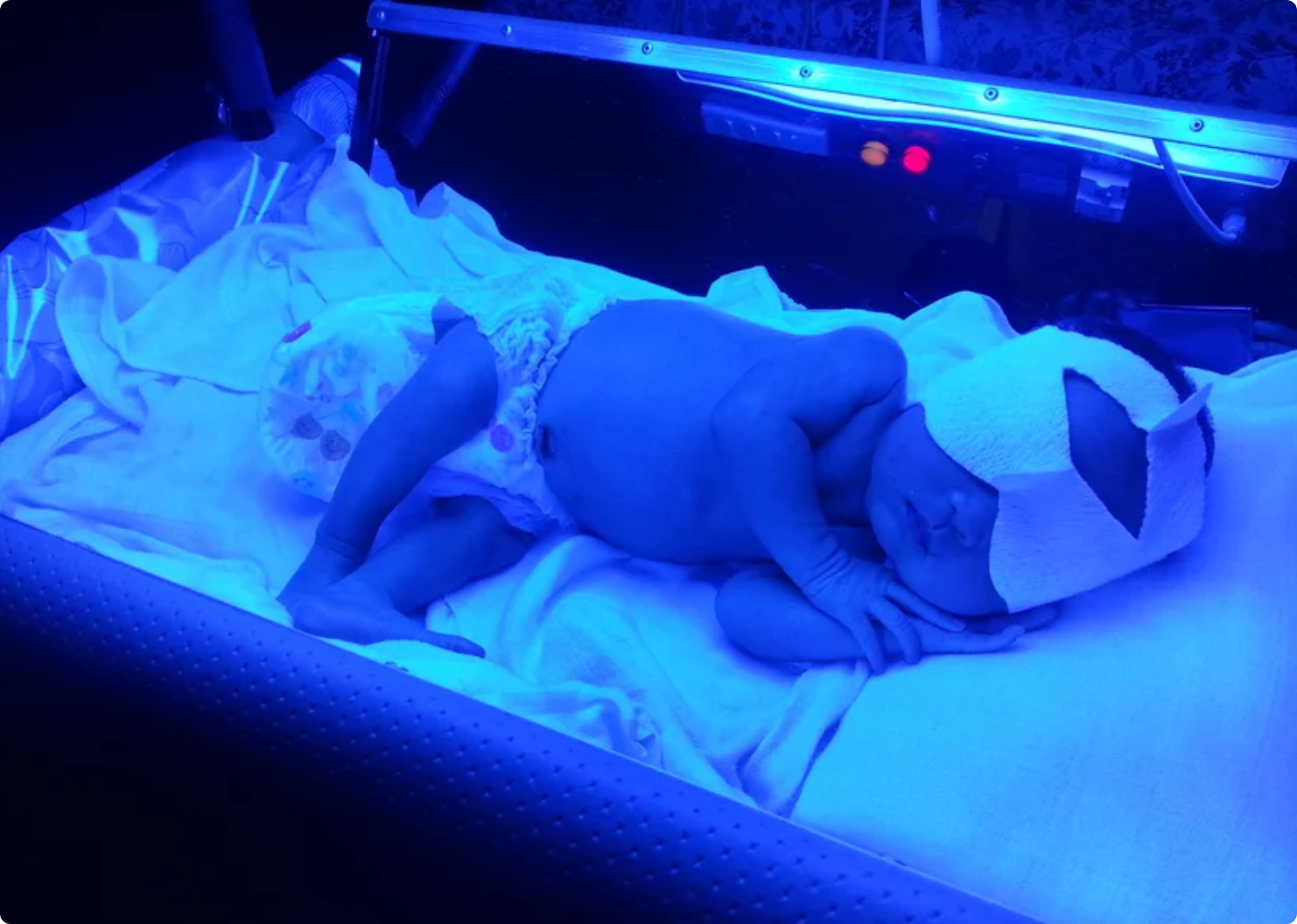
Neonatal Phototherapy
Jean Ward discovered that sunlight helped with the treatment of jaundice. A doctor observed that infants were far less yellow after she’d wheeled them out into the courtyard — a practice she began since convinced the fresh air and sun would do them more good than the stuffy atmosphere of the incubators. Phototherapy was pioneered as as treatment protocol as a result.

The Crash Cart
Anita Dorr invented the crash cart after seeing how long it took for clinicians to gather the essential items needed to address patients in critical condition. With the hope of reducing the amount of patients lost due to this delay, she began prototyping the cart in her basement — sizing it exactly to carry everything used when immediate intervention is needed.
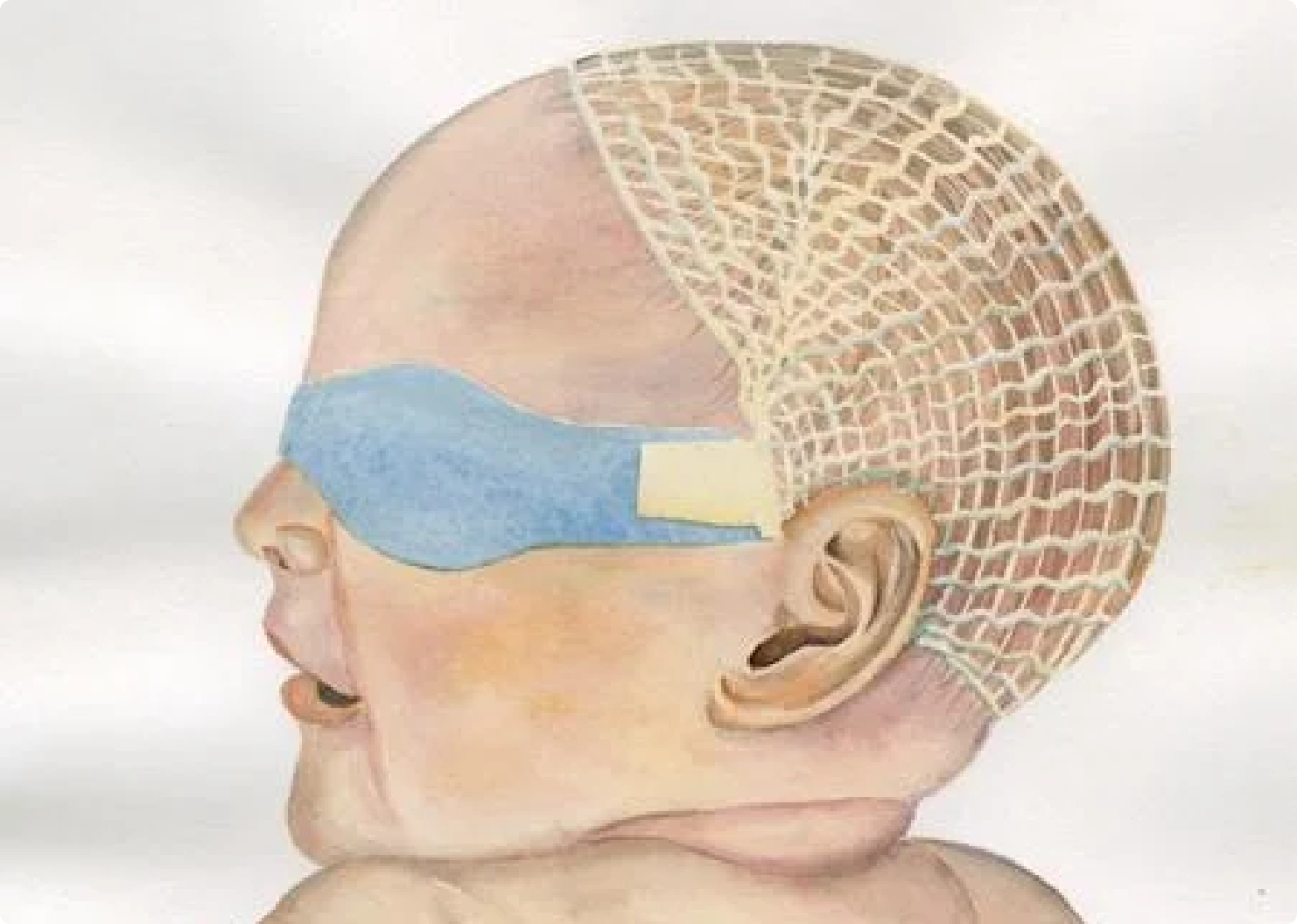
Bili-Bonnet, developed by Sharon Rogone, is currently a product of Small Beginnings, Inc
The ‘Bili-Bonnet’ Phototherapy Mask
Sharon Rogone created a protective mask to fit premature babies being treated for jaundice. Before the Bili-Bonnet, clinicians would often protect a baby's eyes from the bright lights with whatever materials were close at hand — like construction paper and cotton balls!

Color-Coded IV Lines
Nurses Teri Barton-Salinas and Gail Barton-Hay were granted a patent for color-coded IV lines in 2003. This simple yet crucial innovation helps to reduce errors in medication administration and makes time-sensitive infusions easier.
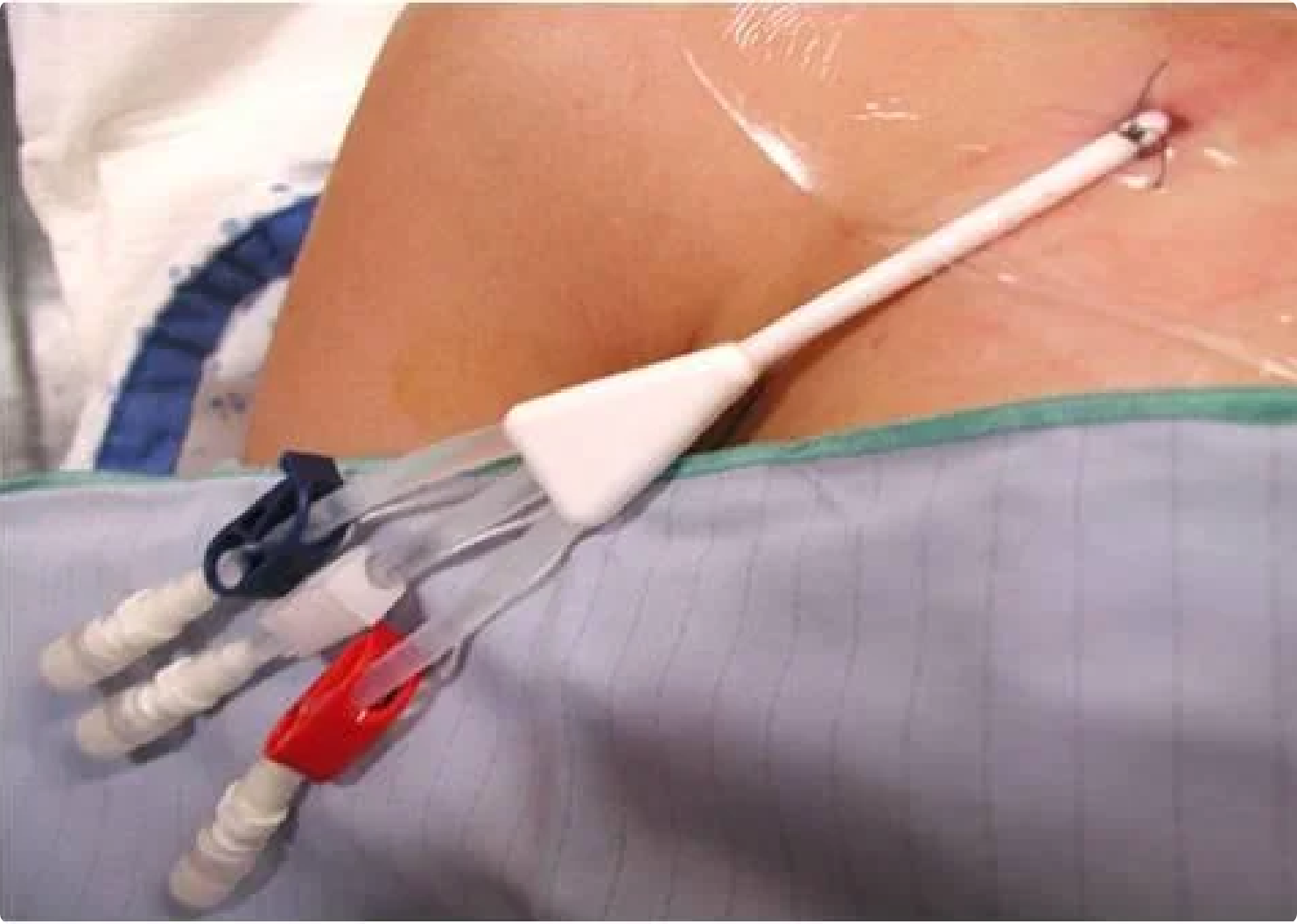
Central Line-Associated Blood Stream Infection (CLABSI) Prevention
Clinicians have played a pivotal role in the prevention of CLABSI and have been the driving force behind advancements like sterile dressing changes, “scrubbing the hub” for 10 to 15 seconds, and protocols to encourage the removal of the central line if certain criteria are no longer met.
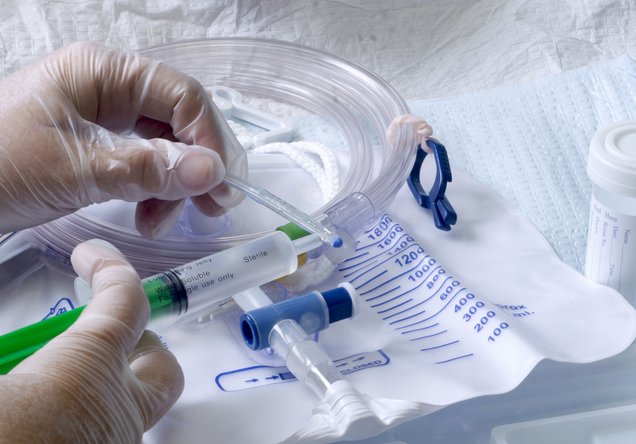
Catheter-Associated Urinary Tract Infection (CAUTI) Prevention
Over the last decade, clinicians have inspired significant progress in the prevention of CAUTIs. For example, they’ve helped develop strict protocols for hygienic catheter placement, leg attachment devices and Foley bag hooks to prevent movement or the collection of bacteria, and urine collection kits to ensure samples are sterile.











%20%5BConverted%5D.png)


The Facts About Pressure Injuries

Hospital Acquired Pressure Injuries on the Increase
New patient safety data for the period 2014–2017 shows that hospital-acquired conditions (HACs) are on the decrease. The report, released in 2019, shows this good news doesn’t extend to pressure injuries, though, which rose by 6%. Read more about it here.

Extended Patient-Stays
Patients without pressure injuries have an average hospital stay of 5 days, while those who succumb to injuries stay an average of 11. This can impact the facility through reimbursement issues, increased risks, and overall costs. More importantly, the patient experience and quality of life is also impacted.

Increased use of Medical Devices
Injuries related to medical devices make up 9% of all pressure ulcers. Often, using these devices are unavoidable. To ensure effective treatment, it’s essential to know which devices can cause a greater risk for injury or breakdown, as well as how we can proactively reduce injury through correct placement on or around the patient.

Decompensation and Acclimation
Extended exposure to moisture and pressure are two key contributing factors to skin degradation in the areas that eventually become pressure injuries. When skin, our largest organ, becomes compromised, it can fail to respond to the additional overload of these factors. Or, it can become acclimated to the consistently repetitive therapies of traditional support surface modalities and fail to respond to that therapy.

Cross-Functional Collaboration of Care
Traditional therapeutic support surfaces and pressure injury treatments struggle to support multiple care disciplines provided by other members of the patient care team, such as Respiratory Care and Physical Therapy. When delivering combinations of treatments, it’s important that pressure injury prevention and treatment doesn’t benefit only one care discipline while presenting challenges for others.

Growing Complexities in Patient Care
With the growing complexities of patient care, healthcare facilities are challenged more than ever with the demands of balancing the increasing acuity of patients, while managing limits on staff, funding and facility resources. Being armed with a greater understanding of physiological response, working to engage the body more effectively, the absence of complicated training and additional staff time requirements allows facilities to have a broader approach to address the persistent, multifaceted challenge of pressure injuries.
The Facts About Pressure Injuries






Hospital Acquired Pressure Injuries on the Increase
New patient safety data for the period 2014–2017 shows that hospital-acquired conditions (HACs) are on the decrease. The report, released in 2019, shows this good news doesn’t extend to pressure injuries, though, which rose by 6%. Read more about it here.
Extended Patient-Stays
Patients without pressure injuries have an average hospital stay of 5 days, while those who succumb to injuries stay an average of 11. This can impact the facility through reimbursement issues, increased risks, and overall costs. More importantly, the patient experience and quality of life is also impacted.
Increased use of Medical Devices
Injuries related to medical devices make up 9% of all pressure ulcers. Often, using these devices are unavoidable. To ensure effective treatment, it’s essential to know which devices can cause a greater risk for injury or breakdown, as well as how we can proactively reduce injury through correct placement on or around the patient.
Decompensation and Acclimation
Extended exposure to moisture and pressure are two key contributing factors to skin degradation in the areas that eventually become pressure injuries. When skin, our largest organ, becomes compromised, it can fail to respond to the additional overload of these factors. Or, it can become acclimated to the consistently repetitive therapies of traditional support surface modalities and fail to respond to that therapy.
Cross-Functional Collaboration of Care
Traditional therapeutic support surfaces and pressure injury treatments struggle to support multiple care disciplines provided by other members of the patient care team, such as Respiratory Care and Physical Therapy. When delivering combinations of treatments, it’s important that pressure injury prevention and treatment doesn’t benefit only one care discipline while presenting challenges for others.
Growing Complexities in Patient Care
With the growing complexities of patient care, healthcare facilities are challenged more than ever with the demands of balancing the increasing acuity of patients, while managing limits on staff, funding and facility resources. Being armed with a greater understanding of physiological response, working to engage the body more effectively, the absence of complicated training and additional staff time requirements allows facilities to have a broader approach to address the persistent, multifaceted challenge of pressure injuries.

A New Innovation to Keep Pressure Injuries in Check


Introducing the Innovative Airisana® Therapeutic Support System
Airisana® was developed to represent a unique, new approach in alternating pressure and microclimate management that would support care teams by combining many of the best practices devised to prevent healthcare-acquired pressure injuries into one device.


1Randomized Pressure Therapy Modes
Traditional therapeutic support surfaces most often use a repeating pressure therapy pattern. A patient’s body easily adjusts to this over time, resulting in adaptation to the surface and a less beneficial outcome. Airisana™ seeks to reduce this risk and promote sustained pressure reduction by randomized pressure therapy modes and programming that combine the benefits of multiple pressure therapies in one surface.


2Microclimate Management
The consistent airflow and whole-body even spread of traditional therapeutic support surfaces can excessively dry or over-cool the patient’s skin where unnecessary. Airisana™ uses unique valve technology to target airflow delivery where the highest pressure is indicated, giving therapy where it’s needed most.


3Easy-to-Use Therapeutic Support
No medical technology helps if it causes more trouble than it’s worth. Airisana™ is easy to clean and simple for staff to transport and store — it’s lightweight and easy to fold. An intuitive soft touch user control unit simplifies patient setup, and is quiet enough to keep the healing environment comfortable and tranquil


4Effective for Comprehensive Patient Care
Interdisciplinary care collaboration, such as respiratory therapy or physical therapy, is essential to apply a wholistic care approach as part of the prevention of and reduction in the risk of pressure injuries or additional acquired conditions leading to an extended hospital stay. Many air surfaces may not safely support bedside therapies without risk. Airisana™ is designed to safely facilitate bedside therapy with stable and supportive side perimeters that are intended to aid in these care activities, rather than standing in the way of the multiple care disciplines one patient often needs. The firm stabilized perimeter and supportive foam base can also make Airisana ready even for emergencies, with a simple, quick access hose connection for disconnection or rapid attachment, as well as a CPR deflate function.


5Turn Assistance and Repositioning
A therapeutic support surface shouldn’t get in the way of hands-on care. Airisana™ was designed to allow care staff to reposition the patient on the surface, while they provide oversight at bedside. This gentle turn is intended to reduce friction and shear risk, as well as prevent staff injuries often associated with the lifting and pulling that accompanies repositioning.


Enhancing Care, Reducing Capital Equipment and Reducing Cost of Care
Even the most effective medical technologies are ineffective when no-one can afford them. Airisana™ desires to returns savings of more than 120% when purchased, compared to the cost of traditional, rented therapeutic support surfaces. When compared with many facilities’ average rental expenses, a return on investment is realized within 2-3 months. Further, the facility may be impacted through reduced reimbursement, increased risks of litigation, and overall costs from managing multiple surfaces and the time to place at-risk patients on a treatment surface.
What Do Pressure Injuries Really Cost ?
Reducing PIs saves more than your patient’s suffering — it also saves money. Use the calculator below to discover the true cost of PIs for your facility or system.
Cost of PI (USD $) treated in your facility
Estimated amount of patients with PI's

*Padula WV, Pronovost PJ, Makic MBF, et al. Value of hospita resources for effective pressure injury prevention: a cost -effectiveness analysis. BMJ Qual Saf. 2018; 0: 1-10. doi:10.1136/ bmjqs-2017-007505
*Russo CA, Steiner C, Spector W. Hospitalizations related to pressure ulcers among adults 18 years and older, 2006. HCUP Statistical Brief. 2008; 64: 1-9. http://www.hcup-us.ahrq.gov/reports/statbriefs/ sb64.pdf. Accessed April 24, 2019.


Try Airisana® and experience the difference firsthand.
Register your facility for a product evaluation.


Try Airisana® and experience the difference firsthand.
Register your facility for a product evaluation.

621 Macon Street
McDonough, GA 30253
Privacy Policy And Terms And Conditions
California Supply Chain Act
© 2024 Encompass Group, LLC. All rights reserved
![]() Proudly made in the U.S.A. by Encompass Group, LLC
Proudly made in the U.S.A. by Encompass Group, LLC








-01.png)
